Australian cancer registry data
An article published today and available free in The Medical Journal of Australia by Louise Gordon of QIMR provides an insight into another aspect of the Australian healthcare system in addition to the controversial issue of out-of-pocket medical costs.
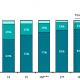
The findings are based on 452 cancer patients diagnosed from Nov 2010- Nov 2011 identified via linkage to the Queensland Cancer Registry. Melanoma accounted for 44% of cases, prostate 25%, breast 19%, colorectal 7% and lung 5%. The costs for medical services and pharmaceuticals were collected for the 2-year period following diagnosis via data linkages with Medicare.
The power of data linkage is clear, but in 2018, how useful is information on services performed prior to Dec 2013?
All cancers, except basal and squamous cell carcinomas of the skin, are notifiable diseases in Australian states and territories. This means there is legislation in each jurisdiction that requires hospitals, pathology laboratories and various other institutions to report all cases of cancer to their central cancer registry.
An agreed minimum data set collected by these cancer registries is supplied annually to the Australian Institute of Health and Welfare (AIHW), where it is compiled into the Australian Cancer Database (ACD). The ACD currently contains data on all cases of cancer diagnosed from 1982 to 2012 for all states and territories, and for 2013 cases for all jurisdictions except NSW.
However, the current data set does not collect any genetic information at tumour-level, and this needs to be addressed urgently to ensure the ongoing value of the data.
Further to this, the introduction of an electronic health record for every Australian, unless they opt out, by the end of 2018 should be the catalyst for an overhaul of the existing cancer registry infrastructure to enable faster availability of collected data to researchers and policy makers.